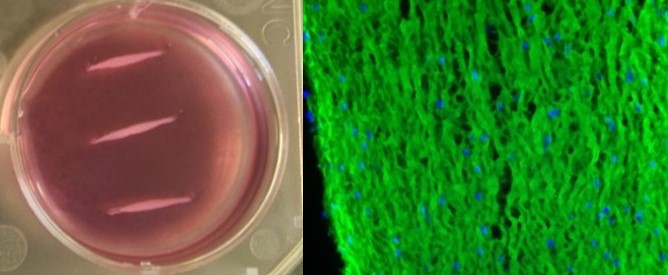
Stem cell based treatments
Novel treatments for tendon injuries in horses
Much of the exploration into new treatment options for tendon injuries in animals has taken place in the horse. Tendon injuries in horses are very common and they heal by forming scar tissue that is pre-disposed to re-injury. Standard treatments for tendon injury (e.g. surgery, ice application, bandage, box rest and controlled exercise, use of corticosteroids and other substances) have not improved the outcome and new treatments are required. Horses also provide a relevant large animal model for human tendon injuries.
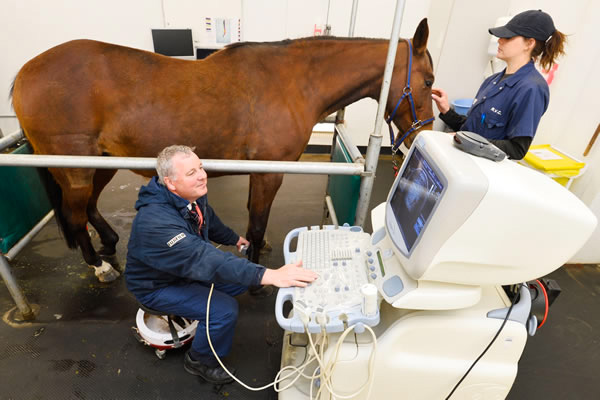
Stem cell-based therapies
The RVC was the setting for the first use of stem cell therapy in horses. Mesenchymal stem cells taken either from the bone marrow or fat tissue can be expanded in the laboratory and used to treat the patient animal from which they were derived.
In comparison with established tendon treatments, mesenchymal stem cell-based treatments have shown improved outcomes, by halving the re-injury rate in both racehorses and sports horses compared to conventional management.
These studies have been performed on a sufficiently large group of clinical cases presenting at equine practices nationally and followed for three years after treatment in order to compare with other treatments with adequate statistical power.
The injury itself only causes pain and lameness for a short period, but when the injury is severe often results in euthanasia because of the poor prognosis for a successful return to performance.
Therefore, in a small number of cases (14 horses), with full consent from owners, horses that were already destined for euthanasia due to a career-ending tendon injury were recruited for stem cell treatment in a much more controlled study conducted under the Animals Scientific Procedures Act (ASPA).
These horses were divided into two groups, where one group received stem cells in their inured tendon and the other group received only saline (control group) in their injured tendon. All horses underwent the same rehabilitation protocol as used clinically for six months at which point they were humanely euthanised and their tendons analysed in the laboratory.
As with any ASPA study, every care was taken to ensure the welfare of the horses recruited.
This experimental controlled study has provided invaluable information on the quality of the tissue of the restored tendon compared to tendons that did not receive stem cell treatment and really adds significant weight to the clinical field observations that this treatment is effective in improving the quality of tendon repair.
Clinical application of stem cells
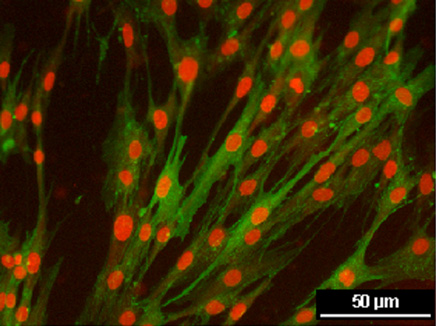
Since 2016 the RVC has been providing mesenchymal stem cells to treat tendon injuries and joint diseases in horses. There has also been increasing demand for stem cell therapies in small animals and the use of mesenchymal stem cells to treat joint disease in dogs has grown in popularity. This has been supported by increasing evidence that stem cells have beneficial clinical outcomes. There has also been a rapid expansion in research to understand how mesenchymal stem cells work.
Mechanisms of stem cell function
Mesenchymal stem cells do not function by turning into tendon cells themselves but via their anti-inflammatory properties. Tendon injuries evoke an inflammatory response, and prolonged inflammation contributes to poor tissue regeneration.
To follow up on our initial in vivo work, we have developed new in vitro models to better understand the mechanisms of stem cell function and the role of inflammation in tendon injury. Using 3-dimensional culture to form “artificial tendons” we have demonstrated that inflammation has many negative effects on tendon cells and have begun to elucidate the pathways which lead to these effects. This work will help us to develop improved treatments for tendon injuries in horses, which may have ramifications for other species such as dogs and humans.