Faecolith in a White Park Calf
Clinical Connections – Spring 2018
James Adams, Staff Clinician in Large Animal Internal Medicine
The Farm Animal Clinical Centre (FACC) was referred a five-month-old White Park castrated male calf who had been dull and depressed for two weeks. The calf had initially been diagnosed with frothy bloat before coming to the RVC.
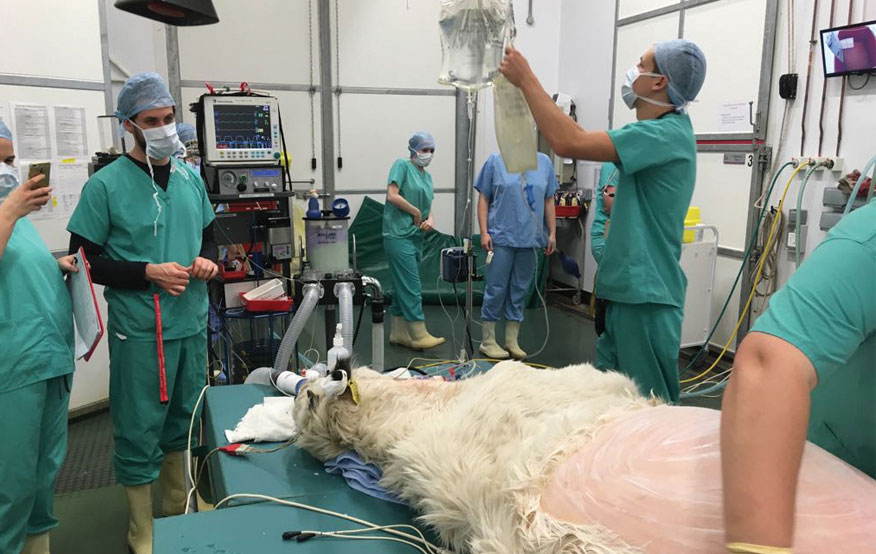
The treatment had not been successful, and a rumenotomy had not solved the problem. There had been no faecal output for a week and he was displaying signs of pain, such as bruxism. The calf presented to the RVC for abdominal ultrasound, with surgery to follow if indicated.
On admission, the calf was reluctant to move, his head was down and he showed no interest in food. He stood with all four limbs placed close together, indicative of pain. The muzzle was dry and the eyes sunken. No rumen turnover or intestinal movement was audible. On rectal examination there was no faeces in the rectum, just some mucoid casts.
A packed cell volume / total protein (PCV/TP) read 44% and 72g/L respectively, and the lactate was 2.9mmol/l (ref range <2 mmol/l), both of which were consistent with the level of dehydration shown clinically. The abdomen was scanned and numerous loops of amotile distended small intestine were seen. The lack of faecal output, distended intestine and the slow progression of the problem all pointed towards an intestinal obstruction.
Mass identified
The calf was given a general anaesthetic and a right paralumbar incision was made midway between tuber coxae and the last rib. The muscle layers were incised and the abdominal cavity entered. The intestines were examined and a firm mass was identified within the lumen of the jejunum. The mass was moved into a non-compromised part of the small intestine where an enterotomy was performed.
An enterolith was removed, measuring 7cm in length and 3cm in diameter. The enterotomy site was closed and the rest of the abdomen explored, where fibrinous tags consistent with peritonitis were seen. The abdomen was lavaged with saline fluid and sutured.
The calf was placed on oxytetracyline to minimise the spread of the peritonitis. The calf is intended to enter the food chain so we were limited in our choice of analgesics, with non-steroidal anti-inflammatories being the only licensed option. Flunixin was given, despite the risk of abomasal ulcers developing in an animal that had not eaten properly for nearly two weeks, and the calf closely monitored.
He initially recovered well from the surgery and was picking at food. On the third day post-surgery the PCV and TP started to drop, which was likely due to an ulcer developing. The calf remained dull and inappetant. He passed black faeces, a typical sign of a non-perforating ulcer. Abdominal ultrasound identified no localised peritonitis typical of a perforating ulcer.
Transfusion
The PCV dropped to 11%, with no evidence of regeneration, meaning that a blood transfusion was needed for the calf to survive. This had an immediate success of increasing the PCV to 16%. Although he had a painful condition we had to stop using Flunixin, as this perpetuated the ulcers. The ulcers needed time to heal.
The calf remained dull over the next couple of days, eating very little. It was another week before he started to perk-up and the PCV and TP increased. Once he started to eat and pass non-tarry faeces he went home, where he made a full recovery.
This case demonstrated the difficulties faced by vets in farm animal practice who are limited by what drugs they can use. The farming industry is leading the way in responsible use of antibiotics, but we as vets have few analgesics licensed in farm species. The case also underlined the importance of knowing all side-effects! On a positive note, this case was a great example of the farm animal team working with both the large animal surgeons and anaesthetists for a successful outcome.
